Three Ways You Can Help Your Aging Loved One
Coloradans are getting older, which means it’s time for families to start thinking about how they’re going to care for their maturing kin. We asked a Kaiser Permanente geriatric psychiatrist for some advice.
When it comes to news about different generations, millennials may garner a lot of the headlines these days, but aging baby boomers increasingly need the most attention. According to the Colorado State Demography Office, the growth of Colorado’s 65-and-older population was third-fastest in the country between 2010 and 2015 — and this population is set to double to more than 1.2 million by 2030.
This means that, pretty soon, a lot of Coloradans will be caring for aging family members — and they’re going to need help. Luckily, there are some things you can do to ensure your loved ones continue to live the happiest and healthiest lives possible, and you don’t become overwhelmed trying to balance the demands of your life and the needs of an aging family member. Jennifer Osborne, MD, is a Permanente geriatric psychiatrist for Kaiser Permanente Colorado and a 2018 Top Doctor. Inspired by her own experiences supporting her grandfather while he navigated the health care system near the end of his life, Dr. Osborne now works with geriatric patients (typically defined as 60 and older, but their ages and overall health status can vary significantly). We asked for her advice on how to best help our loved ones as they grow older. Here are her top three tips:
Be open-minded
There’s no way to know what kind of health issues your loved one will face or what type of medical care they will need as they age. Though the process can be difficult, it’s important to think through various scenarios so you’re prepared for anything, Dr. Osborne says. Possible medical concerns to consider include dementia or cognitive decline, chronic medical conditions, and physical disabilities. “It seems overwhelming to think about,” she adds, but this “helps the patients and those going on the journey with them.”
Talk it out
Instead of being forced to make a critical decision in the midst of a family member’s health crisis, plan ahead. Sit down together and let your loved one outline what he or she wants life to look like in the coming years. “Have conversations ahead of time,” Dr. Osborne says. Create an advance directive — essentially, a plan that outlines your loved one’s preferences regarding medical treatments and care. “Kids could be thinking one way, but then Mom could be thinking a completely different way,” Dr. Osborne says. “Through these discussions, the family can be on the same page.” Some questions to get the dialogue started:
• Where do you want to move if you can’t live on your own at home?
• What do you want us to do if you can no longer drive?
• Who do you want to make your medical decisions if you aren’t able to?
Dr. Osborne and other Kaiser Permanente physicians can help facilitate these important conversations.

Take care of yourself, too
End-of-life care isn’t just difficult for the patient — it’s hard on the family, too. Dementia patients can suddenly begin to behave inappropriately or even demonstrate psychotic symptoms. That can be incredibly hard on those who know them best. “The family might have known Mom or Dad a certain way for many, many years, and all of a sudden they’re different, they’ve changed,” Dr. Osborne says. “It can be a very scary journey.” And it can sometimes leave caregivers feeling overwhelmed.
But it’s not a journey that caregivers navigate alone. At Kaiser Permanente, professionals such as Dr. Osborne work with patients and their loved ones to make the journey as smooth as possible. One of the ways they do this is through the Kaiser Permanente integrated care model. Behavioral medicine specialists are at nearly every Denver, Boulder, and Northern Colorado Kaiser Permanente location, so primary care physicians (PCPs) can include these specialists during a routine exam if the patient and doctor believe it is beneficial. If it is a crisis situation, a crisis team can be called immediately to help manage it. The PCP can also quickly connect with psychiatrists to get any immediate questions answered by phone or direct message.
Kaiser Permanente’s electronic health record (EHR) system is another critical piece to providing the highest-quality care, Dr. Osborne says. In cases where a patient has multiple doctors, but they don’t share medical records, care can be fragmented. But at Kaiser Permanente, “I have all of the pieces of the puzzle that can help me do my job really well. You can have the best doctor in the world, but if they’re not given all of the pieces of the puzzle, it’s going to be really hard to solve.” Whether it’s through personal consultations, telephone consultations, or notes in a patient’s medical records, a truly integrated health care system makes it easy for physicians across specialties and locations to connect with each other and to coordinate patient care.
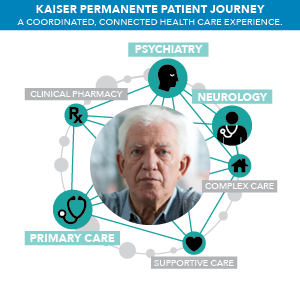
The EHR also helps family caregivers. According to the National Institute of Mental Health, only about half of patients will follow through on making an appointment with a mental health provider. At Kaiser Permanente, a PCP can immediately connect patients or their caregivers to the resources that they need, so no patients fall through the cracks. The EHR also frees the caregiver from having to remember what was said in every doctor’s visit or the names and dosages of each medication their loved one is on because all of that is in the EHR, which tracks the patient across the Kaiser Permanente system. Yet, the caregiver is allowed to access their loved one’s medical records when they are responsible for making care decisions on their loved one’s behalf. This leaves the caregiver to focus on supporting their loved one throughout their care journey. And that means greater quality of life for both the aging family member and his or her caretaker.
Dr. Osborne is among more than 1,200 Permanente physicians serving Kaiser Permanente members across Colorado. Other Permanente physicians who were named to 5280’s 2018 Top Doctors list include:
Matthew S. Koehler, MD-Anesthesiology
Keri J. Propst, MD-Anesthesiology
Jennifer N. Kelloff, MD-Child Abuse Pediatrics
Laurent Lewkowiez, MD-Clinical Cardiac Electrophysiology
Elisa S. Kapler, MD-Dermatology
Barry A. Schoelch, DO-Diagnostic Radiology
Ryan Paterson, MD-Emergency Medicine
Deborah Fromm, MD-Family Medicine
Daniel P. Jones, MD-Family Medicine
Micheline Kuhr, MD-Family Medicine
Jennifer Osborne, MD-Geriatric Psychiatry
Margrit Juretzka, MD-Gynecologic Oncology
Alexander R. Menter, MD-Hematology, Medical Oncology
Frank Becky, MD-Internal Medicine
Lynn L. Rooney, MD-Internal Medicine
Stephen P. Johnson, MD-lnterventional Radiology
Morgan L. Swank, MD-Maternal & Fetal Medicine
Heidi Ray, MD-Neurology
Sirisha Komakula, MD-Neuroradiology
Eric K. Bode, MD-Nuclear Medicine
Jody L. Gibson, MD-Obstetrics & Gynecology
Tyler L. Skaife, MD-Orthopedic Sports Medicine
Timothy R. Muratore, MD-Orthopedic Surgery
Gary L. McDonald, MD-Otolaryngology
David Barclay, MD-Pediatric Anesthesiology
Brian Bagrosky, MD-Pediatric Radiology
Sorenna Kirkegaard, MD-Pediatrics
Sarah Beth Van Scoy, MD-Pediatrics
Edward T. Melkun, MD-Plastic Surgery
Kristy Bauman , MO-Pulmonary Disease
John Christopher Sohayda, MD-Radiation Oncology
John-Paul Morfin. MD-Rheumatology
Walter D. Conwell, MD-Sleep Medicine
David C. Gerhardt, MD-Sports Medicine
Christopher Jockel, MD-Surgery of the Hand
Justin Green, MD-Urology